Your Hospital Experience
Meet our team

The Pre-op Center is where you will first meet our hospital staff. You will have a scheduled appointment approximately 2 weeks prior to your surgery. The staff will interview you and review your medical history, including current medications you take, and provide educational materials as needed. At this time, you will also complete any labs and other tests as ordered by your surgeon.

The Ambulatory Care Unit (ACU) is where you will report on the day of your surgery. Our ACU staff will welcome you and your family, explain your plan of care, and complete the admission processes. They will also assist you into procedural attire, insert the IV, and complete any final pre-operative testing and education.
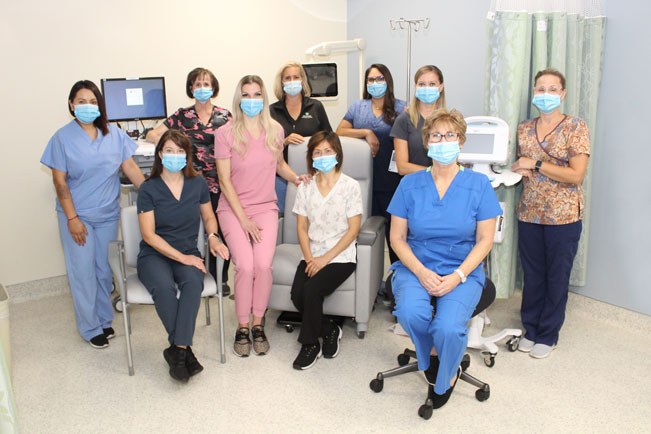
Our Peri-operative Team will take you from the ACU to the surgery holding area, where you will be greeted by our staff and your anesthesiologist. They will review surgical, nursing, and anesthesia plans with you, then you will then be taken into the surgery suite for your joint replacement.
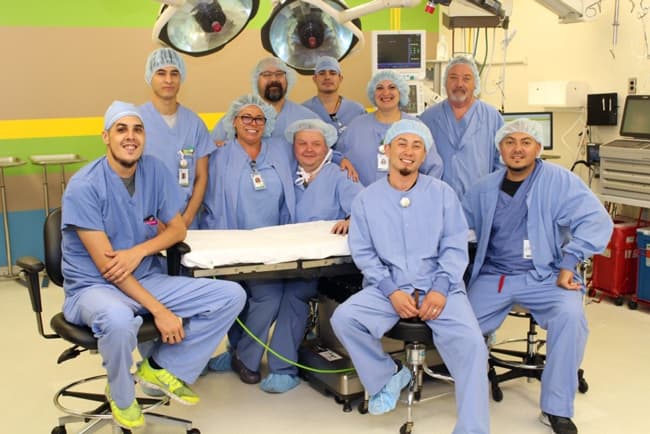
Our PACU Team will care for you in our Post-Anesthesia Care Unit, or recovery room, where you will go after your surgical procedure is completed. The PACU team will monitor your blood pressure, your breathing, and manage pain and discomfort. When all your vital signs are stable, they will prepare the report for safe patient hand-off to the Post-Op team and transport you to the Orthopedic Unit.
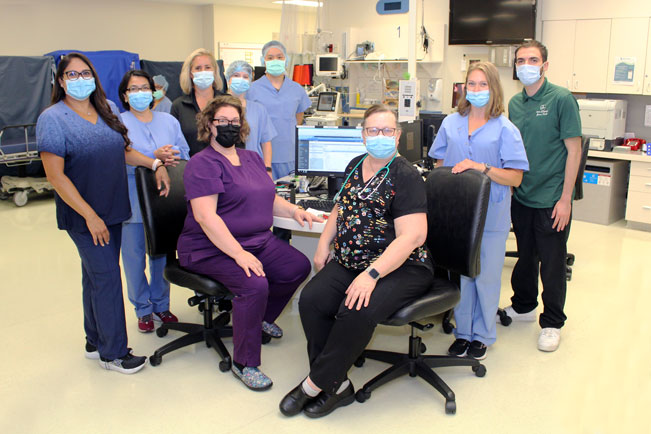
The Orthopedic Unit is located on the 4th Floor of the Vineyard Tower. This unit has:
- 20 designated orthopedic beds (rooms 401- 420)
- Dedicated case manager; physical therapy gym; orthopedic-trained registered nurses, nurse aides, and mobility aides
- Patients are given complimentary active wear to promote health and well-being
- Coaches will be present and participate in physical therapy treatments
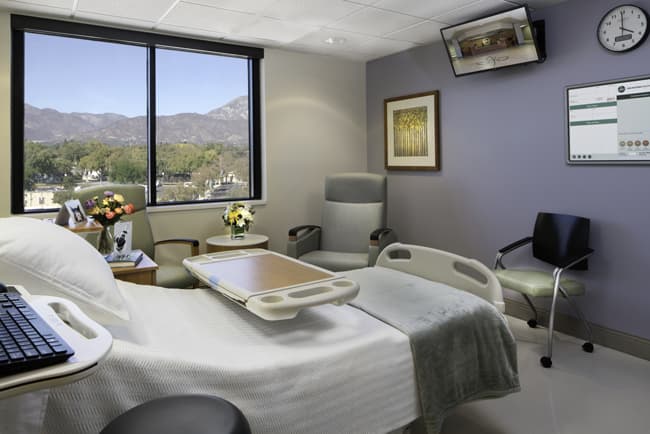
Our Post-Operative Team consists of Registered Nurses, Orthopedic Nurse Navigator, Case Manager, Mobility Aides, and Nursing Assistants. They perform assessments, plan patient care and implement appropriate interventions based on your goals and needs. The team works together to provide comfort and education for you and your coach/family. They ensure that you have any equipment and post-op physical therapy arranged before you are discharged to home.

The Rehab Team consists of physical therapists, physical therapy assistants, occupational therapists, and aides. Their role is to evaluate and establish a plan of care, including realistic functional goals. They will assess and measure range of motion, strength and function as well as educate you and your coach/family on how to safely and correctly perform exercises to enhance strength and flexibility. They will also provide education on any precautions or activities for self-management at home.

Our Support Team consists of pharmacists, respiratory therapists, dieticians, housekeepers, radiologic technologists, and lab technicians. They help to ensure the safety and well-being of our patients and provide vital services throughout the continuum-of-care: pre-op, peri-op, and post-op.

